Spinal Compression Fracture Treatment in Plano, TX
Home > Spinal Compression Fracture Treatment in Plano, TX
Specialties
Expert Vertebral Compression Fracture Treatment in Plano
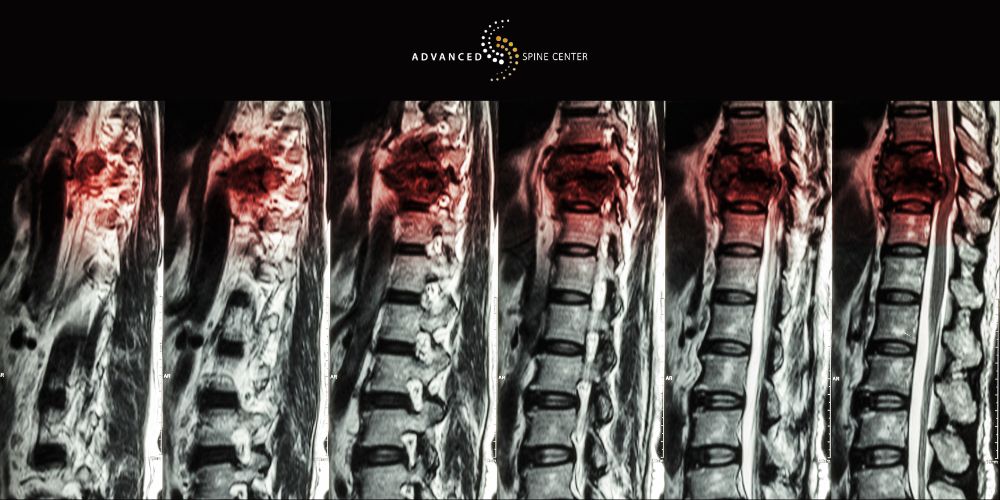
At Advanced Spine Center, we provide comprehensive care for patients dealing with the pain and limitations caused by spinal compression fractures. This type of compression fracture occurs when the vertebrae in your spine collapse, often due to osteoporosis, trauma, or other underlying conditions.
Dr. Stephen Courtney and his team diagnose and treat compression fractures using advanced techniques, including nonsurgical treatments, pain medications, and surgical options such as spinal fusion or bone cement injections. If you or a loved one is experiencing symptoms caused by a compression fracture, call (972) 499-5457 to explore effective treatment options and begin your path to recovery.
What Is a Compression Fracture in the Spine?
A compression fracture in the spine occurs when a vertebra becomes damaged or collapses under too much pressure, either due to weak spine bones or a sudden injury. This type of fracture causes the affected vertebrae to take on a wedge shape, leading to back pain, reduced height, and difficulty performing normal activities.
How Serious Is a Compression Fracture of the Spine?
In some cases, a fractured bone may cause only minor discomfort, while more severe spinal compression fractures can lead to chronic back pain, muscle weakness, and difficulty performing normal activities. If untreated, these fractures can cause permanent deformities like a dowager’s hump, loss of height, and increased pressure on nearby spine bones, increasing the risk of additional fractures.
What Are the 3 Types of Compression Fractures in the Spine?
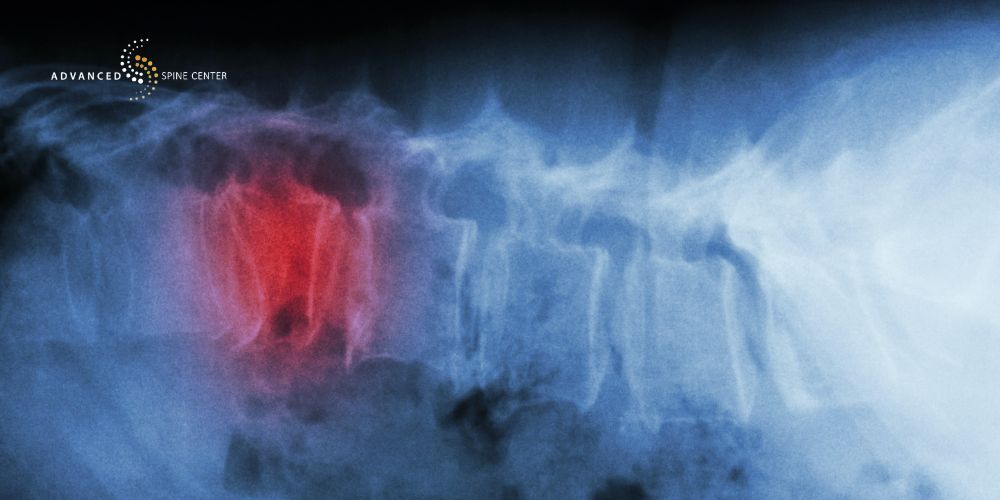
The three types of compression fractures in the spine are wedge compression fractures, burst fractures, and crush fractures. All three compression fractures involve damage to the vertebrae due to too much pressure on the spine bones. These fractures may result from conditions like osteoporosis, traumatic injuries, or other factors that weaken the vertebral body.
Wedge Compression Fractures
Wedge compression fractures occur when the front portion of a vertebra collapses while the back remains intact, creating a wedge-like shape. These fractures are often linked to osteoporosis and are commonly found in the thoracic spine.
Treatment for wedge compression fractures focuses on relieving pain, stabilizing the fracture site, and preventing future fractures through therapies like back braces, pain medications, and bone-strengthening techniques.
Burst Fracture in the Spine
A burst fracture is a more severe compression fracture that occurs when a vertebral body breaks into multiple fragments. This type of fracture is usually caused by high-impact trauma, such as a car accident or fall. It can affect both the spinal cord and spinal nerve roots, leading to neurological symptoms like muscle weakness or problems controlling bodily functions. Because of the potential for serious complications, surgical options such as spinal fusion or bone cement are often recommended to stabilize the spine and prevent additional damage.
Crush Fracture in the Spine
A crush fracture involves the entire vertebral body collapsing and can occur with osteoporosis or trauma. Crush fractures may cause severe back pain, reduced mobility, and an increased risk of additional fractures in nearby vertebrae.
Unlike wedge fractures, which affect only part of the vertebra, a crush fracture impacts the entire structure. Treatment options may include physical therapy, pain medicines, or, in more severe cases, surgical treatment.
Stable vs Unstable Compression Fractures
A stable compression fracture occurs when the spinal bones remain aligned despite the fracture, meaning the spine retains its structural integrity and does not pose an immediate risk to the spinal cord or nerves. These fractures often heal with conservative treatments like rest, bracing, and pain management.
An unstable compression fracture involves significant misalignment or shifting within the spinal column, which can lead to nerve compression, spinal deformity, or even paralysis if left untreated. Unstable fractures often require more aggressive treatments, such as surgery, to restore spinal stability and prevent further complications.
What Causes Vertebral Compression Fractures?
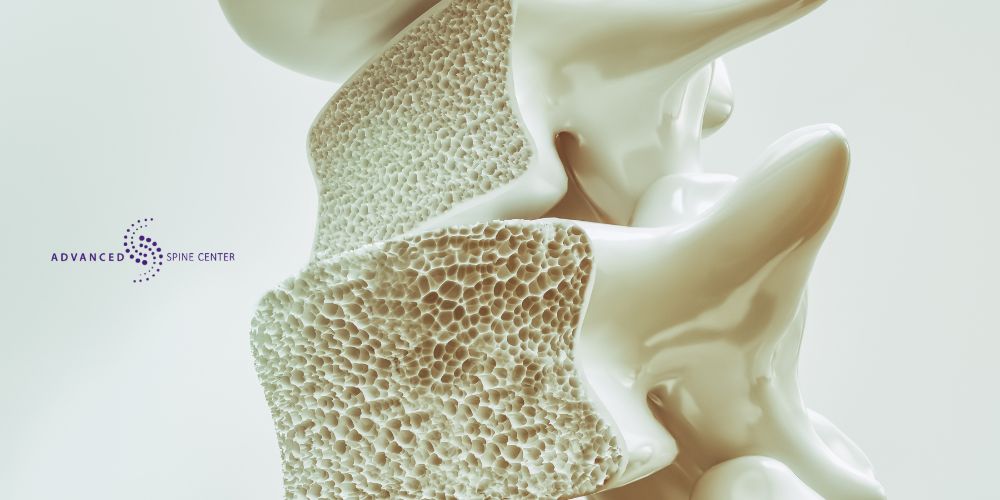
Most compression fractures result from underlying conditions like osteoporosis, which reduces bone density, or from injuries caused by trauma such as a fall or car accident. In some cases, they may also develop due to the presence of tumors that weaken the vertebrae.
For those suffering from vertebral fractures, identifying the cause is essential for determining the most effective treatment plan to relieve pain, promote healing, and prevent future fractures.
Spinal Compression Fracture from Fall or Other Trauma
A spinal compression fracture occurs when the vertebrae in the spine are subjected to a sudden, forceful impact. High-energy accidents, such as car crashes or falls from significant heights, can put excessive pressure on the spine bones, causing them to collapse or shatter.
Osteoporosis
Osteoporosis is one of the leading causes of spinal compression fractures. This medical condition weakens bone density over time, making the vertebrae more fragile and prone to collapse under everyday pressures. This condition is especially common in older adults, particularly women, and can lead to fractures even with minimal strain, such as bending or lifting a light object.
Tumors
Tumors can weaken the structure of the vertebrae, increasing the risk of vertebral fractures. These growths may originate in the spine or spread to it from other areas of the body, causing the bone to deteriorate and collapse under normal pressure.
Common Locations in the Spine for Compression Fractures
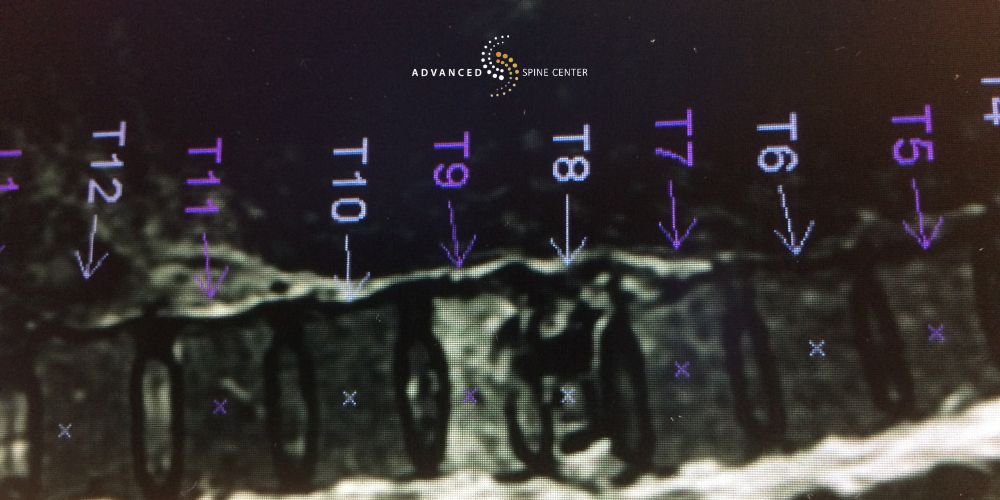
Compression fractures can occur anywhere along the spine, but they are most commonly found in regions that bear significant weight or experience higher levels of stress. The thoracic spine and the upper lumbar spine are frequent sites for these types of spinal fractures.
T11 Compression Fracture
A T11 fracture can cause significant back pain and reduced mobility, as this vertebra is vital in connecting the thoracic and lumbar spine. Treatment focuses on relieving pain, stabilizing the fracture site, and preventing future fractures.
Depending on the severity of the fracture, your doctor may recommend a nonsurgical treatment, such as a back brace or, in severe cases, a spinal fusion to stabilize the fracture site.
T12 Compression Fracture
A T12 compression fracture is common due to the stress placed on this area during activities or injuries. These fractures may cause back pain, difficulty performing normal activities, and even a loss of height.
Addressing a T12 compression fracture often involves a combination of pain medications, physical therapy, and, for severe fractures, surgical treatment such as spinal fusion or bone cement injections.
L1 Compression Fracture
An L1 compression fracture affects the first vertebra in the lumbar spine, which supports much of the body’s weight. This type of fracture is common in individuals with weakened bone density due to osteoporosis or after a traumatic injury.
An L1 fracture can lead to significant lower back pain, reduced mobility, and, in severe cases, impact the spinal cord, potentially causing neurological symptoms. Treatment may include physical therapy, pain medications, or surgical interventions like spinal fusion or acrylic bone cement to stabilize the area.
L2 Compression Fracture
A compression fracture in the L2 vertebra, located in the middle of the lumbar spine, can occur due to weakened bone density or a sudden traumatic force. This type of fracture is often caused by excessive force or weakened bones due to conditions like osteoporosis or tumors. Symptoms of an L2 compression fracture may include back pain, difficulty walking, or muscle weakness.
Depending on the severity of the fracture, treatment options can range from nonsurgical treatments like bed rest and back braces to more advanced procedures.
L4 Compression Fracture
An L4 compression fracture impacts the lower lumbar spine, which bears much of the body’s weight and enables movements like bending and lifting. Fractures in this region often result in back pain, muscle weakness, and difficulty maintaining an active lifestyle.
Treating an L4 compression fracture generally involves pain management, improving bone density through therapies or supplements, and, in severe cases, surgical options such as spinal fusion or bone cement to stabilize the fracture site and prevent further complications.
What Are the Vertebral Compression Fracture Symptoms?

Vertebral compression fracture symptoms can vary, but the most common indicator is back pain that suddenly develops or worsens over time. This pain is usually localized to the area of the fracture and may increase with movement. Other symptoms include a noticeable loss of height, difficulty performing normal activities, and a stooped posture.
In more severe cases, a compression fracture can lead to muscle weakness, tingling, or numbness if the spinal cord or spinal nerve roots are affected. Individuals may also experience decreased mobility or trouble with problems controlling bodily functions, especially if the fracture places pressure on surrounding nerves.
If you’re experiencing these symptoms, it’s important to undergo a thorough physical exam, including imaging tests like X-rays, a CT scan, or a bone density test, to accurately diagnose the condition and determine the best treatment approach.
Vertebral Compression Fracture Treatments in Plano
Advanced Spine Center offers several treatment options for vertebral compression fractures designed to alleviate pain, promote healing, and restore mobility. Depending on the severity of the fracture, your care may include nonsurgical treatments such as back braces, pain medications, and physical therapy to support recovery and strengthen the spine.
When conservative treatments fail to provide relief, surgical intervention may be necessary to stabilize the spine and reduce pain. Minimally invasive procedures such as vertebroplasty and kyphoplasty in Plano, TX involve injecting bone cement into the fractured vertebra to restore its shape and strength. This approach helps prevent future fractures and improves spinal stability.
If the vertebral body is significantly damaged, spinal fusion surgery may be performed to permanently stabilize the spine by fusing two or more vertebrae together. These surgical options can significantly reduce pain and improve the quality of life for patients with severe compression fractures.
Our team takes a personalized approach to care, often incorporating strategies to address underlying issues like bone loss or osteoporosis, including bone density exams and nutritional guidance to improve bone strength.
Recovery from Spinal Compression Fractures

While mild cases of compression fractures often improve with nonsurgical treatments like pain medications, back braces, and physical therapy, procedures such as vertebroplasty or kyphoplasty can help stabilize the spine and may speed up recovery. On average, most compression fractures heal within several weeks to a few months, though recovery times may differ depending on the individual.
Life Expectancy After Compression Fracture in the Spine
Life expectancy after a compression fracture in the spine largely depends on the patient’s overall health and the cause of the fracture. For individuals with osteoporosis, managing bone density and preventing future fractures are crucial for maintaining long-term health.
While a single fracture is not generally life-threatening, untreated fractures can lead to complications such as chronic back pain, loss of mobility, and increased risks of other health issues.
Life Expectancy After Compression Fracture in Elderly Patients
A compression fracture can impact health and mobility in elderly patients. While many recover with proper care, the condition increases the risk of complications such as loss of independence, decreased activity levels, and future fractures.
Addressing the fracture quickly with treatments like pain medications, back braces, and bone-strengthening therapies is key to preventing further health decline.
What Are the Long-Term Effects of Spinal Compression Fracture?
Common long-term effects of compression fractures include chronic back pain, reduced height, and changes in posture. Persistent pain and limited mobility may also make it difficult to perform normal activities, contributing to a decreased quality of life.
Untreated or severe fractures can increase the risk of future fractures and put strain on surrounding spine bones, leading to further complications. If the fracture affects the spinal cord or spinal nerve roots, nerve-related issues like tingling, numbness, or problems controlling bodily functions may occur.
Can You Make a Compression Fracture Worse?
Yes, a compression fracture can worsen if not properly treated or if excessive strain is placed on the spine during the healing process. Activities like heavy lifting, bending, or twisting can increase pressure on the fracture site, potentially causing the vertebrae to collapse further. This can lead to heightened back pain, more severe deformities, and an increased risk of future fractures.
Contact the Advanced Spine Center in Plano for Treatment of Spinal Fractures
At Advanced Spine Center, Dr. Stephen Courtney and our dedicated team offer advanced treatments to address spinal compression fractures, relieve pain, and restore mobility. Whether you’re seeking relief from persistent symptoms or looking to prevent future fractures, we’re here to help.
Call (972) 499-5457 to schedule a consultation and explore your treatment options for lasting recovery from compression fractures.


